Friday 11/13/2020
I went for a short walk. A resident has prepared a table of all the walks starting at Channing House to local destinations, with their exact mileage, and Lenny, who is now managing the resident website, put it online. So I walked from CH to the gazebo in Gamble Gardens and back, 1.5 miles. That nicely filled the time until it was time to go to Stanford Hospital to meet Dr. Watkins, who placed my aortic stents.
It was a trace emotional, driving down into the underground parking and walking past the reflecting pool to the main hospital building. That was a trip I made at least 30 times, maybe 50, while Marian was undergoing a series of procedures back in 2018; and I hadn’t made that trip since. (For my own recent procedures I was in a newer building and didn’t drive and park.) Anyway after filling out a form and answering some questions for the nurse coordinator and the nurse practitioner, Dr. Watkins herself entered the room. She’s not quite as dramatic looking as I remember her from last month, but still a big, tall woman, maybe 40? (could be a bit younger but not a lot, to be an experienced surgeon) with lots of red-brown hair, a pleasant face, and thick nerd glasses. She was quite generous with her time, for a busy surgeon, giving me at least 20 minutes of discussion on all sorts of things, during which she made these notes:
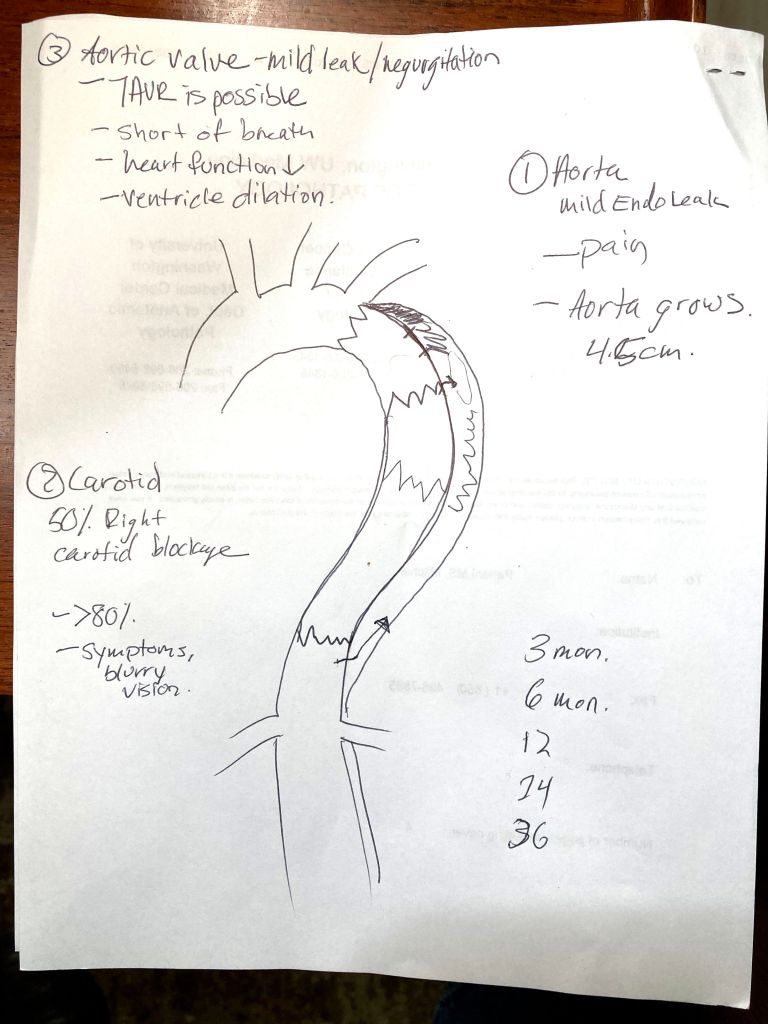
First, the aorta. The wiggly lines are the ends of the overlapping wire stents. The bulge on the right is the aorta wall, with its split-off lining inside. The space between the lining and the wall proper is full of blood and starting to clot and will eventually be resorbed by the body. However there are currently a couple of “endo-leaks” (small arrows) where blood is seeping past the stents into the “false lumen”, the space between the lining and the wall.
She expects they will stop and clot also, when I stop taking Plavix (clopidogrel), the anti-clotting med that caused my recent endless nosebleed. And here I learned something: that drug is prescribed for six months following a cardiac stent, and is not needed by the aortic stents in the picture. Remember back during my first hospitalization, as part of clearing the floor for the aortic work, they did a catheterization of my heart and found one artery 80% blocked, and more or less on the spur of the moment, placed a stent? That one. Because of that stent, I’m on Plavix for six months, to March. When I go off it, the “endo-leaks” in the aortic lining should clot up.
We’ll know because, see the stack of dates lower right? Those are the call-backs for CT scans and re-checks. If the endo-leaks don’t clot up, she says there’s a very simple procedure where she goes in with a catheter and inflates a balloon to smush (I think she used that word) the lining outward. Not even full anesthetic, and discharge the next day. Very confident, like all surgeons. Other things to watch for in later scans: dilation of the aorta. Currently it is stable at 4.5cm (see right side of notes), dilating further would be a problem.
The big question raised by Dibiase was, with all that hardware in the aorta, could the complicated catheterization of the TAVR procedure be done? Good news. Dr. Watkins said cheerfully, “Oh yes, I can scoot a TAVR right up there, no problem.” And went on to point out that she does most of the TAVR’s in her group. So that resolved that question.
Then we talked TAVR and she got up the CT scan to check a few things. An experienced person can basically fly through the CT image like a drone, turning through all dimensions. At some points I could see my ribs as a line of ovals, so I was looking in from the left side, and then she swung it around and there were ribs as curving bars so we are looking out or down or something.
Anyway, she looked in detail at the aortic valve. “See the circle of bright dots? That’s the stitching around the valve seat.” The CT didn’t resolve the leaflets in really high res, but she could see maybe a little gap in one that might account for the current regurgitation. But her take was that my valve looked “great”, and it could last “three to five years yet”. She said she looks at a lot of aortic valves when evaluating TAVR prospects. The way the prosthetic valves usually fail is that they get calcified and stiffened, which shows up clearly on the CT. Compared to the usual TAVR candidate, my valve looks pristine.
One caveat, though. She asked if it was a cow or a pig valve. Pig, I said. “Ah. Well, there is one kind of porcine valve that doesn’t get calcified, but just fails anyway.” So there is that uncertainty. Things to watch during the 3/6/12 month scans are listed in the upper left of the notes. In particular, if the valve gets very leaky, the left ventricle tends to dilate in size, which would show up on either a CT or an echo.
We also talked about the carotid arteries because Dr. Dibiase had heard something that didn’t sound right in my neck. Watkins pointed out that in a pre-op carotid echo, the analysis noted one artery had a 50% velocity increase, which usually indicates some kind of blockage. However (see lower left of notes) this is not usually a problem until an 80% blockage. Things to watch for: any neural symptoms, especially episodes where your vision gets blurry for a brief time and then recovers. People tend to brush that one off but it means carotid insufficiency.
Later in the day we had Rhonda’s weekly meeting, which was mostly good news. In particular for the 2nd or 3rd week in a row, we have zero COVID cases. She shared the official guidance on holiday gatherings that was just released by a consortium of ten Bay Area counties. You know the drill: max three households, outdoors, masked, and short. No fun. What’s the point?
Wow(!) what a detailed efficient report…all good news I am assuming?!
Yes the Holidays are cancelled at our house- we can’t take a chance to gather all around our table-especially when half the group don’t follow pce rules- the governor is putting us all back in the box again. As the covid is getting so much worse-
Thank God Bill still has a job- I haven’t worked at all this year-
Hope you continue to heal and stay healthy- sending you my love….laurel
LikeLike